How does chronic pain after hernia surgery occur?
Chronic pain after inguinal hernia surgery occurs in approximately 5-15% of patients. The main cause of pain after hernia surgery is mesh placement near nerves. Since 1987, mesh repairs have become much more prevalent due to their advertised decrease in hernia recurrence. Indeed, for most surgeons who perform 50 or less hernia repairs each year, the recurrence rate will be less when using mesh, as opposed to non-mesh hernia repair options.
With a traditional mesh repair, the mesh is placed on the outside of the abdominal wall to patch the hernia defect from the outside (anterior mesh). There are three nerves, the ilioinguinal, iliohypogastric, and genitofemoral nerves, that run along the outside of the abdominal wall in the same location as this mesh. When a sheet of mesh is placed or sutured near or to one of these nerves, the result is often significant pain that begins immediately after surgery.
Most of the patients that we see in our office who suffer from Chronic Groin Pain complain of severe pain in the recovery room after hernia surgery that never subsides. We feel that there is a clear relationship between the location of the mesh placement and the incidence of chronic pain. This is why we recommend a posterior mesh repair, as it avoids these nerves and results in a much lower incidence of chronic pain.
Is there an issue with the mesh plug?
We also see patients that complain of a hard mass in their groin and have pain from a mesh plug that was inserted into the internal opening of the inguinal canal (internal ring). As can be seen in the picture here, taken during during laparoscopic surgery, the mesh plugs not only block the hernia opening, but constantly put pressure on the surrounding areas. As you can imagine, this patient experienced chronic pain after his hernia surgery.
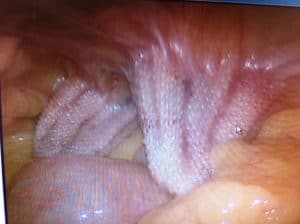
Mesh plugs from inguinal hernia causing chronic pain
Are non-mesh hernia repairs better?
Non-mesh hernia repairs have the distinct advantage of not leaving a large piece of mesh against nerves. However, the trade off is that there is a higher incidence of the hernia coming back over time (hernia recurrence). One of the confounding factors about non-mesh repairs is that they are generally only performed by high volume hernia surgeons, and likely have better results because they are performed by hernia specialists rather than the average general surgeon who performs many different types of operations.
Why are posterior – preperitoneal – hernia repairs better?
Recent data has shown that posterior mesh repairs – advanced open preperitoneal repair, laparoscopic or robotic have a lower incidence of chronic pain than the traditional mesh repairs. This is intuitively obvious since the posterior repairs avoid 2 out of the 3 common nerves entirely, unless a fixation tack is used. For the past 20 years Dr. Reinhorn has performed over 5,000 of the posterior mesh repairs with a minimal incidence of chronic pain.
He first performed these under general anesthesia using sophisticated laparoscopic equipment and later learned how to do the same repair without the need for general anesthesia and through one small incision in the groin. Dr. Fullington is an experienced laparoscopic hernia surgeon who has also been extensively trained in the same approach thought the small groin incision. It is important to learn what your unique options are by speaking with a qualified hernia doctor.
About Dr. Reinhorn & Dr. Fullington
Dr. Michael Reinhorn is a specialist in inguinal hernia and umbilical hernia. He started his practice as a general surgeon in 2001, and in 2012 he transitioned to focus on the care of hernia patients. In 2018, he co-founded Boston Hernia, an ambulatory surgery practice focused exclusively on hernia surgery. In 2020, Dr. Nora Fullington was recruited from her work as a general surgeon, where she performed hundreds of laparoscopic hernia repairs, to Boston Hernia where she was intensively trained by Dr. Reinhorn in the open preperitoneal and Shouldice techniques. Together with their physician assistant team, they perform approximately 800 hernia surgeries every year. Both surgeons offer a tailored approach for each patient, taking into account individual patient factors to decide if surgery is recommended or not, what type of repair (open, laparoscopic, mesh, non-mesh) is best, and what type of anesthesia is safest. At Boston Hernia, our focus is on each individual patient and continuously improving our own surgical techniques and outcomes. We do this by participating in various hernia societies, studying our own outcomes through a national database, and publishing our data to influence the care of hernia patients nationally and internationally. Boston Hernia is an affiliate practice of the Mass General Brigham system. In addition to operating at Newton-Wellesley Hospital, a Mass General Brigham Hospital, we offer care at ambulatory surgery centers in Waltham, MA and Derry, NH.