By guest author Move Strong PT
Disclaimer: these are some suggested exercises to start with when dealing with a groin injury. Every injury is different and a thorough physical evaluation by a physical therapist is needed.
Sports related & work related groin and lower abdominal pain can be a frustrating and perplexing problem. It has been dubbed by some as the “Bermuda Triangle” of musculoskeletal injuries. The complexity arises from the wide range of structures that can contribute to this issue.
The muscles of the inner groin and the lower abdomen attach closely to each other, and work together to stabilize the pelvis. For this reason, groin injuries usually involve a dysfunctional relationship between these structures, not just a problem in the area that hurts.
Thankfully, some headway has been made in our understanding of how to diagnose and manage these injuries. After reading this blog, you will have a better understanding of the steps that you can take to recover from sports related groin pain.
Make Sure Its a Groin Strain
First it is important to identify the source of the pain. There are a number of medical conditions that can refer pain to the groin, such as an inguinal hernia or testicular cancer. In addition, hip, low back, and nerve injuries can refer pain to the groin. Consulting with a sports medicine orthopedic surgeon, or a specialist such as Dr. Michael Reinhorn of Boston Hernia can help you to rule out any serious medical conditions.
If your pain is in fact due to a sports related groin injury, the next step is to address the contributing factors.
Risk Factors
Determining the risk factors of a groin injury guides our treatment. Some are not within our control, such as:
- Shape of pelvis
- Sport of choice (high prevalence in soccer and hockey)
- Previous Injury

(https://performancephysio.ie/groin-pain-differentiation-in-athletes-doha-agreement/)
There are other root causes that we can control. These are:
- Overuse
- Suboptimal mechanics
- Stress
Stress is such an expansive topic that we will not go in depth for this blog – but realize that it has a massive impact on any injury and must be considered. Here is an introduction to understanding the balance between stress and recovery.
Overuse
Overuse, or repetitive strain, can occur both in the short term (acute) or the long term (chronic).
Acute overuse happens when the strain on your body exceeds what it can handle in a short period of time. Did you start a CrossFit program 4 times a week or an advanced running program after a year of no activity? These behaviors significantly increase the risk of injury.
Chronic overuse happens when the strain on your body exceeds what it can handle over a long period of time. Does your rigorous sports schedule leave little time for recovery? Do you play one sport year round at a young age? This strains the same areas of the body over and over again, when the body thrives on variety to distribute stress.
This highlights the importance of gradually increasing your tolerance to physical activity, and listening to your body for feedback.
Suboptimal Mechanics
When engineers design machinery, they consider mechanical advantage. They put things in a position to create a large force from a small input.
Think of how much easier it is to lift a vehicle with a car jack.

(https://haynes.com/en-us/tips-tutorials/how-work-under-your-car-safely)
The principles of mechanical advantage also apply to the human body.
Muscles attach to bones, and operate best when these bones are aligned a certain way.
Groups of muscles pull against each other to stabilize the body. In the case of the pelvis, the lower abdominal and groin muscles interact in this manner.
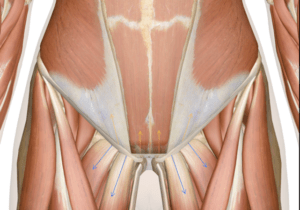
https://www.innerbody.com/anatomy/muscular/lower-torso
If certain muscles are at a disadvantage because they are not positioned well, they will have to work a lot harder to do their job. For example, if the pelvis is stuck in an excessive anterior pelvic tilt, the abdominals and hamstrings will be stretched and in a less optimal position.
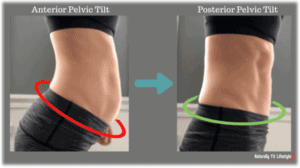
(https://www.naturallyfitlifestyle.com/a-guide-to-postpartum-hip-realignment-with-pelvic-tilting/)
Sometimes our pelvis is shifted towards one side of their body. This leads to one set of groin muscles working more than the other side.
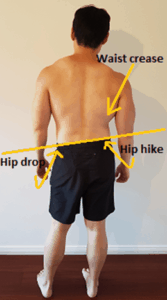
(https://posturedirect.com/lateral-pelvic-tilt/)
To make matters worse, as these muscles fatigue, your brain will call on other muscles to help out. This will take away the ability of the extra muscles to perform other tasks. Overall this creates stability, but sacrifices freedom of movement due to stiffness.
Ultimately, this can result in decreased adductor strength and hip range of motion, both of which are risk factors in developing an adductor related groin injury.
If muscles are overworking because they are out of position, the total strain on them is greater. If poor mechanics and overuse are both present, the risk of injury becomes much higher.
Classification of Sports Related Groin Injuries
A physical therapist will perform a series of tests to rule out any contributions from the lumbar spine, hip, and/or nerve related injuries.
They will then assess your hip/abdominal strength and range of motion in order to classify the injury. Different tests will correspond to different muscles, and help to determine the focus of your rehabilitation.
According to the Doha agreement, sports related groin injuries can be classified in 4 ways:
- Adductor-related groin pain
- Iliopsoas-related groin pain
- Inguinal-related groin pain
- Pubic-related groin pain
(Weir et al 2015, Doha agreement meeting on terminology and definitions in groin pain in athletes. https://bjsm.bmj.com/content/49/12/768)
Usually individuals fall into a single category, and adductor-related groin pain is the most common. It is not uncommon however for someone to have symptoms belonging to more than one of these areas.
Your PT will also test functional movements related to your activity/sport of choice in order to track progress. These may include single leg balance, squats, and jumping, depending on the severity of injury.
Treatment of Sports & Work Related Groin Injuries
Treatment should focus on the following:
- Managing pain
- Improve tissue tolerance
- Improve mechanics
- Functional/Sport Specific training
Managing Pain
Isometrics are often effective at decreasing pain. The following are parameters you can follow for performing isometric exercises.
- Imagine you are turning up a dial that controls the intensity, starting your contraction at 0% and then to 10%, 20%, and so on. Max 70% intensity.
- Increase the intensity until you get to the point of MINIMAL symptoms, or the sense that you are at the limit of what is safe.
- Hold for 20-45 seconds
- Rest 1 minute
- Repeat for a total of 2-5 sets
- 2-3 times a day
- If symptoms are worsening, you are squeezing too hard and should turn down the dial a little bit.
The following are isometric exercises you can do, depending on the type of sports related groin injury that you have. Click Here for a PDF document.
Adductor-Related Groin Pain Isometrics

Iliopsoas-Related Groin Pain Isometrics
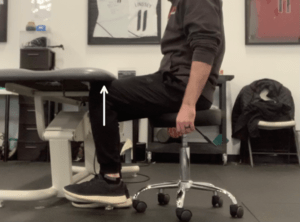
Inguinal-Related Groin Pain Isometrics

These circular arrows represent a posterior pelvic tilt. Two ways you can create this motion are by flattening the lower back/tucking your tailbone, or by pulling your belt buckle towards your chin. The muscles that rotate the pelvis in this direction are the abdominals and the hamstrings. In this particular case, we are focused on activating the abdominal muscles.
Foam Rolling
Foam rolling can decrease pain, increase blood flow, stimulate cellular healing, and decrease muscle tone. Use the following guidelines to include this in your rehabilitation. Click Here for a PDF version.
- Lightly roll over the muscles in the specified areas
- Spend 20-30 seconds on each
- If there is a particularly tender area
- pause and maintain pressure
- perform slow exhalations (6 seconds each)
- wait until the tenderness subsides (max 3 minutes)
- Adductors

- Quads

- Hip Flexors

Improve Tissue Tolerance
After pain is under control, improving tissue tolerance becomes the focus.
Your injury can be re-aggravated if you do too much. Conversely, you won’t stimulate improvements in resiliency if you don’t do enough. Tissues need tension to remodel and heal well.
In short, doing the right amount is best.
Using a pain scale can be helpful to determine the appropriate exercise and intensity of injured tissue.
A general rule of thumb is to consider pain from 0-2 to be safe, and 3 to be a zone of caution in tendinopathy. Anything above a 3, and the exercises need to be regressed in some manner.
Track pain levels during the following, careful to keep pain from exceeding a 3/10:
- While performing exercises.
- The hours after exercises.
- The day after exercise. It should not exceed levels of discomfort that you normally experience.
The following are examples of beginning progressions for 3 of the categories of sports related groin pain. (For Pubic-related groin pain, consult a physical therapist for a plan of care.)
Start off performing these exercises every other day, 3 x 8 repetitions. Reps should be done slowly, with a 3 second eccentric (lowering) phase.
Adductor-related groin pain
Side-lying Adduction
Adduction with band
Modified Copenhagen
Iliopsoas-related groin pain
Half Kneeling Hip Flexion
Standing Hip Flexion
Standing Hip Flexion with Band
Inguinal-related groin pain
Supine Marching
Short Lever Side Planks
Supine Kettlebell Pullovers
Click HERE for a PDF version of these exercises.
Improve Mechanics
The hamstrings, glute max, and glute medius all must be operating effectively for optimal mechanics of the pelvis. Here are some exercises you can do for each of these. Include these exercises with any of the classifications of sports-related groin pain. Continue to use the pain guidelines from the Tissue Tolerance section.
Hip Abduction (against wall)
Bridge w/ Adductor Squeeze
Hamstring Posterior Pelvic Tilt
Progress to 9090 Hip Lift with Shift (to activate adductors)
As long as these exercises are not too taxing, you can do them 4-5 times a week. Eventually, you will be working these muscles in a general strengthening program.
Improving limitations at joints in other areas of the body, such as the ankles or mid back, can improve efficiency up/down the chain at the pelvis. Having a movement specialist help you to identify your problem areas can facilitate your progress.
Functional/Sport Specific Training
Eventually training needs to involve functional training, namely hip stability. The following are examples of functional exercises that eventually would be appropriate to progress to.
For each of the following, use the pain guidelines previously mentioned.
Start with 3 x 8 and if appropriate, choose a weight that provides a 7/10 difficulty level.
Slow Eccentric Split Squat
Hip Airplanes
Lateral Squats
Sport specific training will be highly individualized for the athlete, depending on their activity of choice. The demands on a soccer player are much different than those on a baseball pitcher, and their training should reflect this.
At Move Strong Physical Therapy in Hudson, MA, we work closely with the strength and conditioning coaches at Cressey Sports Performance. We recommend that our clients recovering from sports related groin injuries eventually shift to a well designed training program. Returning to sports and other physical activities should be a smooth transition, in order to reduce the risk of re-injury. Good strength coaches are experts at facilitating quality movement, reducing the risk of re-injury, and increasing performance.
How Physical Therapy Can Help
Physical therapists are trained to assimilate all of this information and tailor a program to fit your needs.
Specifically, they will help with:
- The diagnosis and classification of your injury
- Manual therapy techniques to manage pain and speed up recovery
- Soft tissue and joint mobilization
- Instrument assisted soft tissue mobilization
- Dry needling
- Assessing and improving movement quality
- Managing workload
- General strengthening and conditioning
- Sport specific training
Often these injuries will heal with a 3-6 month course of physical therapy and follow up training. Unfortunately there are times when sports-related groin injuries do not respond to conservative treatment, and more invasive procedures are the appropriate next step. But if you do not address the factors that contributed to the injury in the first place, then you may end up with the same problem all over again.
Here is a downloadable PDF summary of Category Specific Groin Pain Exercises
If you have questions, or would like an evaluation from an expert physical therapist contact
This blog is not a substitute for medical advice. If you are experiencing symptoms, consult a licensed healthcare provider.

