I’ve been meaning to write this blog for probably about 15 years now. so, what’s kept me waiting?
Surgical thinking vs change management
A lot of reasons. I tend to jump to conclusions quickly. The beginning of my career as a surgeon was focused on obtaining relevant information in the fastest and most efficient manner to make a timely decision that could sometimes mean the difference in a patient’s survival. I’ve learned over my 22-year surgical career to take my time and get as much information as possible before coming to conclusions. This is a useful skill when outside the operating room or outside an acute surgical setting and is critical when trying to change an organization or to change the mindset of the surgical community.
Recognizing patterns in inguinal hernia repair early
It was obvious to me twenty years ago, as an ex-engineer, that repairing hernias should involve sound engineering and physics principles. When possible and safe, mesh should be used and placed on the inside of the abdominal wall, where the abdominal pressure is pushing the mesh into place against the abdominal wall, as opposed to the most common repair where mesh is placed on the outside of the abdominal wall and pressure pushes the mesh away from the hole that it’s repairing. We now have overwhelming data to support this statement (Stabilini et al 2023), but this data was not available 20 years ago, and this principle was not widely accepted by the surgical community. My work for the last 20 years has allowed us to collect data and finally publish outcomes that help us understand the big picture better.
Missed opportunities in hernia surgery
Over the last 20 years, recalls for medical devices, specifically mesh, have led to public distrust in mesh implants. Next followed the massive push toward transparency and patient safety. The result is a push to improve medical devices, which in some cases has been helpful and, in other ways, has inappropriately directed blame at the mesh device and ignored the surgeon’s role in causing harm. Multiple lawsuits directed at the mesh implant have created fear and misinformation. In my opinion, this has led to a missed opportunity to improve outcomes and properly educate patients on the risks and benefits of mesh.
A patient’s journey with chronic pain after inguinal hernia repair
I will tell a patient’s story and tie that back to the beginning of this blog. About 8 years ago, a patient and his wife came to me because he had suffered permanent disability after inguinal hernia surgery. Another surgeon had attempted to repair his hernia, but the hernia repair failed almost immediately. After going in for a second surgery with his original surgeon, the patient woke up with severe pain and disability related to a nerve injury that had not been corrected through numerous attempts over a year and a half. This patient was nearly suicidal and in tears in my office, looking for help. Because there were no experts in chronic pain after hernia surgery in the Boston area at the time, I offered to remove two of his nerves and repair a recurrent femoral hernia that was missed in the first two operations. This patient ultimately improved. According to his report, he got more than 80% relief, but he never regained full quality of life compared to before his initial hernia surgery. I’ve kept in touch over the years with this patient and have shared with him my experience in better understanding anatomy and working to improve patient outcomes at the initial hernia repair and prevent chronic pain at the outset.
I learned hernia anatomy AFTER my surgical training
In 2012, I did a double neurectomy on a patient who had experienced chronic pain after inguinal hernia surgery. In hindsight, I had a limited understanding of the nerve anatomy of the groin despite having performed over 1500 hernia repairs in the first 10 years of my practice and having completed 5 years of surgical training in Boston. While doing a chart review a few years later, I read my own operative note where I mentioned removing the ilioinguinal nerve and a “second nerve that was more medial.” Despite being considered an expert, I was completely unaware of the name of the iliohypogastric nerve in 2012 and how to identify it during surgery. This is not a unique situation. Surgical trainees are consistently taught by surgeons who lack knowledge of this nerve anatomy. Eventually, through independent study, I learned how to identify these nerves in every surgery. It wasn’t until 2016, when I had the opportunity to observe and scrub into surgery at the Shouldice Hospital, that I learned how to identify the third nerve – the genital branch of the genitofemoral nerve on the floor of the anterior inguinal canal. I’ve talked at length about my visit to Shouldice Hospital, as those two days have changed the trajectory of my career. As a result of that visit, I have made it a mission for the remainder of my career to help surgeons learn inguinal anatomy and avoid chronic pain.
I am not alone
In 2019-2021, I had the pleasure of training my friends Ben Poulse and Mike Rosen in the Shouldice repair. Both surgeons are international leaders in the field of abdominal core health and hernia surgery. It was only after their visit to our operating room, that they learned how to identify the genital branch of the genitofemoral nerve as well as a trick to identify the iliohypogastric nerve more easily. In addition to performing safe surgery with a consistent awareness of nerve anatomy and location, they have been reliably performing and recommending the Shouldice repair to dozens of patients yearly and teaching it to future surgeon leaders nationwide. All of us learned this anatomy well after our formal training concluded.
Hernia mesh is rarely the problem (except plugs)
I’m going to rock the boat a little here. To the best of my knowledge (and that of many well-researched and informed scientists), polypropylene is a relatively inert, hydrophobic material that has been used safely for sutures and mesh implants for over 70 years with minimal problems. These days, hernia mesh is most commonly made out of polypropylene. Millions of pieces of polypropylene mesh are implanted into the citizens of the United States yearly, and tens of millions are implanted throughout the world each year just for hernia surgery alone. Yes, there are many variables that will contribute to a patient having a poor outcome when having hernia surgery. In the US, 85% to 90% of patients have a good outcome when having a mesh repair, an almost identical percentage of those having a no-mesh repair. The mesh does not increase your risk of having a bad outcome. Given these numbers, it is very unlikely that the mesh is the source of the problem. So what is the biggest source of poor outcomes after inguinal hernia surgery?
It is the surgeon!
My story: I spent 15 years learning hernia anatomy after completing my surgical training in Boston. I traveled to multiple states and countries to learn nerve anatomy and techniques. The leaders of my field were in the same boat. There is limited inguinal/groin nerve anatomy education across the board for surgeons in training and this lack of knowledge carries through into practice after training. This suggests to me that the problem is not the plastic implant but the technician placing the implant in the human body.
How did we get here?
I will backtrack to 1994 when I was a third-year medical student at Cape Cod hospital. I remember a medical device sales representative being in the operating room giving a surgeon a piece of polypropylene mesh plug and telling him to “just shove it in the hole”. In two separate cases, an umbilical hernia repair and an inguinal hernia repair, I watched as a medical device sales rep told a surgeon how to do a case. Over the following several years, I watched device reps guiding surgeons to “shove” multiple plugs in multiple holes in both the groin and the umbilicus. I didn’t know any better at the time, I was a medical student and surgical resident. I relied on attending surgeons to tell me that this was a ludicrous way to fix a hernia, but they didn’t. Medical device salespeople convinced them this was a safe and appropriate repair method. Surgeons were told that this was a great way to fix a hernia. They could do surgery faster, and patients had less pain because less work was done. Surgeons in the 1990s bought the sales pitch hook, line, and sinker. These surgeons then trained the current generation of surgeons, myself included.
Surgeons lost credibility
The unfortunate outcome of the aggressive sales tactics in the 80s and 90s was that surgeons stopped learning and teaching hernia anatomy, especially in the groin. They just started plugging holes. Patients were, and still are, getting hurt as these plugs brush up against and compress nerves and other structures in the area. Hernia repairs were failing as mesh was pushed out from its intended location by normal abdominal pressure. These plugged holes became unplugged. Surgeons and lawyers invented new terminology to explain complications. “Mesh migration” is one example of an invented term. The mesh doesn’t migrate, it is either placed correctly and used properly, or it is used improperly. The plug is (and, in my opinion, always has been) a horrible product that should not be used. The plug was designed to function similarly to a drywall anchor. In theory, when placed in the space behind the muscles (preperitoneal space), the hope was that the abdominal pressure would “flatten” the plug, keeping it in place. In reality, the plug does not flatten and instead, bunches up like a bullet, and normal abdominal pressure just pushes it out of its intended location. Surgeons and lawyers call it “migration”; I call it an ineffective product and poor surgical technique. If I sound like I’m blaming surgeons, I am, partially. I’m blaming them for falling prey to aggressive marketing and sales tactics by some medical device manufacturers. We have seen this time and again throughout the history of surgery, and we are seeing it continue through this present day.
The lawyers have not helped fix the problem. Instead, they have incorrectly placed blame on ALL mesh instead of focusing on the marketing tactics used by some medical device manufacturers and surgeons’ responsibility to know the anatomy and assess the safety and effectiveness of a product before implementing its use. The class action lawsuits have distracted the public away from the root cause of chronic pain, which is the inadequate anatomical and surgical knowledge in today’s surgeons and trainees. Of course, this is also a byproduct of the aggressive tactics used by some medical device companies. As a caveat here, not all medical device companies are created equal, and I have seen many follow the science and data before recommending new techniques and technologies to the general public.
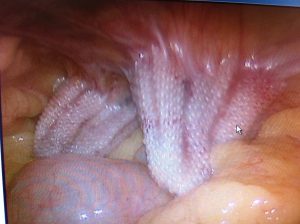
Image of two mesh plugs used to “repair” a right inguinal hernia taken at the time of a laparoscopic appendectomy I performed in 2015. The plugs are poking at the small intestine and the appendix behind them.
Healthy debate, based on data, is critical to moving forward
A paper that we recently published compares the open preperitoneal hernia repair with the Shouldice repair. Mike Rosen and I have debated the findings and how to interpret the data. From his perspective, the fact that patients who get a no-mesh inguinal hernia repair have nearly as good a quality of life at 30 days and a year as patients who get mesh suggests that there is not a lot of benefit to a mesh repair. His take is that a no-mesh repair is a wonderful fix for a hernia. I get it. It makes sense. I look at this data in the setting of repairing over a thousand hernias a year in our practice. We repeatedly see how patients who have an open placement of posterior mesh recover quicker, with less pain, and a better quality of life in recovery. We hear how the no-mesh repair hurts more. All in all, both groups do really well, but the data confirms our observations that there is a difference between how patients recover after surgery, and thus I am more likely to recommend a mesh repair for those looking to have the fastest recovery and best quality of life outcomes.
An important caveat to the above: only a subset of our patients are candidates for a no-mesh repair. This is based on many factors and requires an evaluation by an expert to determine each individual patient’s surgical options.
The big picture of inguinal hernia surgery and mesh
I think the most important bit of information from this paper is the fact that, in experienced hands, we have demonstrated that mesh is good; in fact, it’s a little better than no-mesh. So, all of the arguments from lawyers saying that mesh is bad fall by the wayside when you have experienced surgeons. We cannot blame the mesh for poor patient outcomes. The take-home message from this paper is that we need to educate our surgical workforce on proper inguinal hernia anatomy. We should focus on the basics and not just on the newest and most expensive implants, devices, and robots that have promised to make things better. Surgeons need to evaluate technology critically and, MOST importantly, master anatomy. New technology is just helping us maintain the status quo, which is injuring patients at an alarming rate. It is unacceptable that between one and three patients out of 100 in the US who have an inguinal hernia repair are injured during surgery, leading to long-term disability (Reinpold 2017).
Eradicating chronic pain together through improved surgeon education
By 2021, it was obvious to me that I needed more help, and I had to prove that what we were doing at Boston Hernia was replicable. I had to prove that better outcomes were possible through training in anatomy and surgical techniques. Dr. Nora Fullington, an experienced general surgeon, joined our practice in May of 2021. We spent the first few months together in the operating room, assisting one another on every surgery. We calibrated our technique for open preperitoneal inguinal hernia repair. In this technique, a flat piece of mesh is placed under all the abdominal muscles through a very small incision in the groin, avoiding general anesthesia. The end result is an excellent long-term success rate with near elimination of chronic pain. Over the last 3 years, Dr. Fullington has become a master of this repair and teaches it to a national audience. Her outcomes and my outcomes are identical, proving that great outcomes can be reproduced with education alone. Dr. Fullington has become a champion of the mission to virtually eliminate chronic pain as a complication of inguinal hernia surgery. Our hope is to find additional partners who can help us bring this same level of education to more surgeons, paving the way to eradicating chronic pain after inguinal hernia surgery in the same way we eradicated common bile duct injuries.
Summary
Overall, mesh implants are good for patients. The use of mesh, in experienced hands, reduces the risk of hernia recurrence and is quite safe. Few remaining implants, like mesh plugs, may harm patients and should be avoided. Non-mesh repairs can be good alternatives for qualified patients who want to or should avoid mesh for technical reasons. Lastly, the most important variable is the education, skill, and experience of the surgeon performing the hernia repair. We need to focus more on teaching hernia anatomy, and specifically nerve anatomy, to eliminate the alarmingly prevalent problem of chronic pain.
